Dr Fiona Dignan is a consultant in haemato-oncology and has been clinical lead for haematology at Manchester Royal Infirmary since 2015. She undertook her haematology training at The Royal Marsden in London and developed a research interest in post-transplant complications. Fiona spoke to Billie in Patient Services about the effects of graft versus host disease.
Can you briefly explain the differences between acute and chronic GvHD?
Acute GvHD tends to occur in the first few months following a stem cell transplant and it tends to affect three main organs of the body - the skin, the gut and the liver.
Chronic GvHD tends to occur months or maybe even years after the transplant. It can affect any organ of the body, but it most commonly affects the skin, eyes and mouth. Common symptoms include skin rashes or thickening of the skin, dry and gritty eyes and a painful mouth.
What can patients expect if they experience acute GvHD?
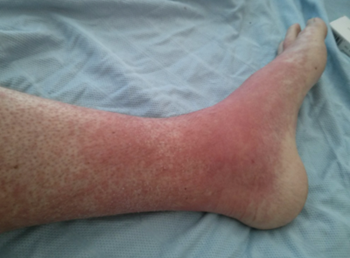
In terms of acute GvHD, the most common thing that we see is a red skin rash that looks a little bit like sunburn. Classically, it starts on the palms and soles of the feet, but really, it can happen anywhere on the body. It can be itchy and it’s sometimes painful.
Along with a rash, some patients are affected in their gut as well, which means that they experience diarrhoea. Most patients find this is relatively mild, but for a minority of patients, it can be quite severe with frequent trips to the toilet. Patients with severe diarrhoea need to be readmitted to hospital for fluids and other medications to help treat the GVHD.
Liver function tests can also be abnormal but this is usually picked up in the clinic. Occasionally patients may notice a yellowish tinge to their skin or eyes if they have liver GVHD.
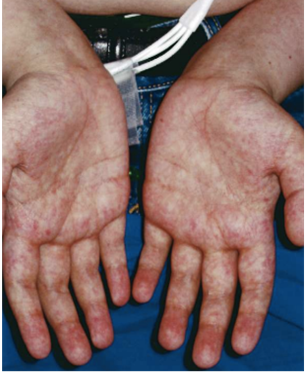
'In terms of acute GvHD, the most common thing that we see is a red skin rash that looks a little bit like sunburn.'
What can patients expect if they experience chronic GvHD?
In terms of chronic GvHD, the most common thing patients would notice are skin rashes, and there are a couple of different types that can happen. There’s one that’s more like eczema - very red, dry and flaky skin. Then there is another type called sclerodermoid GvHD, where the skin becomes thickened, and much tighter. This can lead to restriction of movement in the skin which can, in turn, lead to restriction of movement in the joints.
Another thing that patients sometimes experience is GvHD in their mouth. This usually causes pain or dryness in the mouth. Patients often find that toothpaste stings, and it can also mean that hot drinks and spicy foods are harder to tolerate. Painful ulcers can occur in the mouth too.
Sometimes, along with skin and mouth symptoms, patients can experience changes in their eyes, including dryness and grittiness.
If a patient thinks they have GvHD, why is it so important that they report it to their transplant centre as soon as possible?
Because early treatment can help to get on top of the symptoms and it can also limit the amount of GvHD. So it’s definitely worth contacting the transplant centre for an assessment so we can help as much as possible.
Patients are often told that some GvHD is a good thing, which I can imagine might sometimes be confusing, can you explain why that is?
A bit of GVHD can be a good thing because it shows us that the donor’s immune system is working really well. We know that if the donor’s immune system is working well, it’s probably fighting off the disease too. This is called the graft vs disease or graft vs Leukaemia effect.
So a bit of GvHD is a good thing as it means the disease is less likely to come back, but of course it’s a balance between the good effects of stopping the disease coming back and the difficult symptoms that can arise in having GvHD.
What are the treatments for GvHD, and does this differ for acute and chronic versions?
There are some similarities between the two. For relatively mild GvHD, it can sometimes be managed with topical agents, which means creams or ointments for skin GVHD. These treatments can include moisturising creams and soap substitutes like aqueous cream and oilatum, as well as steroid creams.
In more moderate GvHD, it’s common to prescribe steroid tablets for both acute and chronic manifestations of GvHD.
If the GVHD starts when patients are still on their cyclosporine medication the dose might be increased so that the levels become therapeutic again and this alone might be enough to help treat it.
Can you tell me about ECP treatment?
Steroids, plus or minus ciclosporin, tend to be the first line of treatment in treating GvHD. There are second line options for patients who do not have a good response to steroids and the most common is ECP which stands for Extracorporeal Photopheresis. Nobody knows exactly why this works but it appears to switch off the process of GvHD over time.
Patients undergoing ECP treatment for chronic GVHD usually attend a centre on two consecutive days every fortnight. Sometimes the treatment will be within their transplant centre, but sometimes it will be at a another centre with the expertise to undertake the procedure. ECP is undertaken more frequently for acute GVHD.
ECP involves removing blood using a special machine and treating it with ultraviolet light and medication before reinfusing it back to the patient. The process exposes the white cells in the blood to the ultra violet light and combined with medication, can reduce the effect of GVHD over time.
It’s a very safe treatment and the main side effect that patients mention is tiredness. It is, however, a big time commitment as it’s two consecutive days every fortnight, and on average patients will need the treatment for at least 6 months. After that time, there tends to be a reduction in visits.
Is it available to most patients?
It is available to most patients either at their transplant centre or at another centre with the expertise to deliver the therapy.
If patients develop chronic GvHD, how likely is it that this will resolve in time?
It can be quite difficult to predict whether chronic GvHD will completely resolve. In many patients it does, with steroid and other treatments given over an extended period of time.
For some patients, it can continue with a mild level of symptoms, and then there are a small group of patients who continue to have significant and severe symptoms of chronic GvHD, and in that group it can unfortunately last months to many years after transplant.
You’d consider the most severe, long lasting cases to be a minority of transplant patients?
It is a minority.
Are there parts of the body affected by GvHD that might not be talked about as much, but that patients should be aware of to look out for changes?
Yes, and one to mention is genital GvHD. It’s probably a far more common occurrence than we think as it often goes unreported.
In female patients, having genital involvement is more common if they have skin or oral GvHD. Early referral to a gynaecologist can be quite helpful to get advice on topical treatments.
The gynaecologist can also be helpful in making sure patients have cervical smear tests done, which can be sometimes difficult to do in patients who have vaginal GvHD.
It can also affect the genitals in male patients too. Again, it can be helpful to have the expertise of urology specialists early on.
A less common manifestation of GvHD is in the joints, but it does occur, either on it’s own or sometimes joint movement can be restricted due to tightening of the skin. It’s certainly worthwhile for patients to report any joint limitation, as there are a couple of quick tests doctors can do to see how much the joint movement is restricted.
We know that patients with chronic GvHD can develop other problems because they are on long term immunosuppression, can you explain a bit more about those problems and why they might occur?
The problem that comes with most immunosuppressant drugs is an increased tendency to get infections. These can be common bacterial infections, like chest infections, respiratory virus infections, or urinary infections. But sometimes we see more unusual types of infections like fungal infections or other things that are relatively rare.
The most commonly used drug to treat chronic GVHD is steroids. Unfortunately, while steroids are a very useful drug, the do have a number of side effects. These include muscle weakness, particularly in the upper parts of the legs and arms. This can make getting up from a chair, walking long distances or getting up a flight of stairs more difficult. Steroids can also cause raised blood sugar, raised blood pressure and sometimes severe mood swings.
Being on steroids can also cause thinning of the bones and stomach irritation, so patients find that they are also on a lot of other medicines to protect their gut and their bones, and protect them against infections etc. That can be quite frustrating, especially if they’ve just come off post-transplant medication when GvHD occurs.
'ECP involves removing blood using a special machine and treating it with ultraviolet light and medication before reinfusing it back to the patient. The process exposes the white cells in the blood to the ultra violet light and combined with medication, can reduce the effect of GVHD over time.'
There must a huge psychological strain of living with permanent body image changes as a result of chronic GVHD? How might these patients be supported?
There is a huge psychological impact. One possible avenue of support is if the transplant centre has their own psychotherapist or psychologist. At the Manchester Royal, we are lucky to have both. Usually the Clinical Nurse Specialist in transplant centres can help to arrange referrals to them.
Another line of support that is sometimes available are patient support groups for people who have been through a similar experience, or have similar issues.
In patients that have very particular skin problems and are struggling with their change in body image, it can sometimes be helpful to refer them to a dermatologist or skin specialist. There are some clinics, although only in certain areas, that specialise in skin camouflage creams which can be useful to patients with pigmentation concerns.
Would there be any advice that you can give these patients on managing their symptoms and quality of life?
In terms of managing symptoms, it is really important to take the medication including creams, eye drops and mouth washes regularly. Although it’s quite time consuming to do, it can help cut down the other medicines that might be needed.
It’s also really important to take care of yourself, and it can be really helpful to keep up with other things where you can. Like exercise and catching up with friends. It can improve your quality of life between what can be a gruelling schedule of clinic visits. And doing some regular exercise in particular helps to counteract some of the effects of the drugs, including steroids.
This is presumably because people can gain quite a lot of weight if they are on prolonged steroids?
Yes they can, and also, exercise really helps with muscle weakness and building up some strength.
When you say exercise, if people’s movement is limited due to their symptoms – what do you mean?
I mean any regular movement. Walking is ideal. If walking is difficult outside, then even doing a little bit of walking in the house is beneficial. Some patients find exercise bikes or pedal machines can help to keep them moving and gain muscle strength.
Knowing who will get GvHD is difficult, in terms of research are we any closer to predicting this pre-transplant?
Not really. It’s still difficult to predict with any level of certainty who is going to get it and who isn’t. But it’s definitely an area of active research.
Do you think that advances are being made in the treatment of GvHD?
Yes, I do! There are many more drugs being tested in clinical trials that in the past. These include ruxolitinib, ibrutinib and azacitidine.
Why the change?
I suppose part of the reason is that we are transplanting more patients than ever before, and that means we are seeing more GvHD and so trying to understand it as best we can. This is because we are able to offer stem cell transplants to older patients due to the reduced intensity conditioning option now available.
Another reason could be that it has been difficult to undertake trials in the past due to small numbers of participants, but there is definitely more enthusiasm to find solutions, which can only be good news for patients.
