Ruth, a teacher from Yorkshire, received a stem cell transplant in 2016 after being diagnosed with acute myeloid leukaemia (AML). Ruth has shared her transplant experience, and why she is so passionate now about improving post-transplant care.
Find out how you can get involved with Anthony Nolan’s work to improve post-transplant care by sharing your own experiences in our survey at the end of Ruth’s blog.
For me, the hard part wasn’t the six rounds of chemotherapy, the transplant, the visit to ICU. No, it was, and still is, right here right now. The being on your own all day, everyone saying how well you look, people forgetting to call or text to check in. Assuming you are well because you are back at work or at home; you are far from well, you are literally getting by.
The ups and downs of recovery
After receiving my donated stem cells, all I had to do was wait for my immune system to come back and the transplant to do its thing.
Everything was going to plan, although I couldn’t tolerate the first anti-rejection drug so that was altered. I was told after about eight weeks that I was well enough to go home. I was so excited, I was texting friends and family telling them all the good news.
It was short lived excitement unfortunately, and the next day things started to take a turn for the worst. I started struggling to breathe, I was moved rooms closer to the nurse’s station (that is never a good sign). This was the early stages for acute GvHD (graft versus host disease – your new immune system thinks all of you is an alien and tries to take over you and attack you as well as the illness).
What was happening was my body was starting to hold fluid. I had a heart scan which showed that fluid was building up around my heart which was stopping it being able to beat correctly. This was causing me pain and stopping me from getting oxygen around my body. I needed an operation ASAP to reduce the fluid around the heart.
Just before they did what they had to do, I asked the surgeon ‘was I going to die?’ he responded, ‘we are trying our very best to keep you alive’. At this point, it hit me, this is serious, and I thought, ‘I’ve come this far. I’m not going to die’.
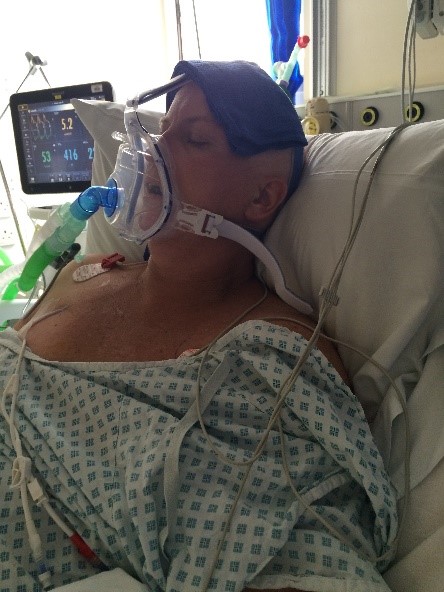
Ruth in hospital
The operation was successful, and I had to spend five days in ICU with tubes coming out of me in all directions. The fluid build-up unfortunately meant I lost my left lung, the fluid squashed it so badly that it wasn’t able to re-inflate. I knew there was a reason for having two lungs! Two weeks later I was on my way home with many, many drugs - enough to open my own pharmacy!
The side-effects of my transplant
I’m doing incredibly well. Though I do unfortunately have chronic GvHD. Basically, my new donor cells are a little too excited – they’re not just attacking the leukaemia, they’re also attacking me.
Because of my transplant and the GvHD, the following is going on: my eyes don’t work correctly and are drying out, so I have my tear ducts plugged to keep the fluid in my eyes; my hands and feet don’t work correctly, the nerves are damaged so I can’t do fine motor skills too well and my feet are in constant pain; my mouth is disintegrating so I don’t produce saliva and I struggle with tasting food. There are many other issues, but I won’t bore you with them!
Using my experience to help others
I am just two years post-transplant - something that the consultants never thought I would achieve - so I have to remember that sometimes I need to give myself a massive pat on the back. I have also been married a year, and I have been back at work as a teacher for the last twelve months. Part time, but back at work.
In July 2017, I contacted Anthony Nolan. One thing led to another and I took part in a campaign called ‘Who Cares?’ which was all about post-transplant care and how no patient’s recovery should be made more difficult by a lack of care and support.
I shared my experience of leaving hospital, and how I felt I was all alone - more or less dropped from a great height and left to deal with it. Part of this campaign was visiting the House of Commons in November 2017 where I spoke to MPs to help raise awareness of why post-transplant care is such a vital part to people’s recovery.

Ruth, Vice-Chair of Expert steering group
Steering post-transplant care forward
In April 2018, Anthony Nolan asked if I’d like to be part of an Expert Steering Group looking at how to improve the pathway for people going through transplant once they leave hospital. I am currently the Vice-Chair of the committee – I feel incredibly strongly and passionately that the whole person needs to be cared for and not just the illness.
The illness is easy, it’s visible, people see it and they care. The after effects, the emotional side-effects, the GvHD, the effects on the family – this is what people don’t see and that’s what’s so hard about this disease. This for me is the biggest weakness of all the treatment I have received and am receiving.
How I’m doing now, two years post-transplant
I have been fortunate enough to have been to the House of Commons twice to help raise awareness of post-transplant care, Vice-Chair the steering group with Anthony Nolan, and had articles printed in national magazines to raise awareness of this illness. I try to think it’s about making good things out of potentially horrific situations.

Ruth with her dogs
The final image is me today - the day I reached two years post-transplant, the day I was told I wouldn’t see!
Ruth’s story highlights some of the physical, emotional and practical challenges that patients can face after a stem cell transplant – but we know that every patient has a different experience, and that’s why we want to hear from you.
If you or a family member has had a stem cell transplant, we’d like to invite you to share your opinions on what the best post-transplant care looks like by answering our survey before Friday 2 November 2018.
Your answers will support our work to ensure that every patient has access to the care and support they need, no matter where they live.
If you’d like more information about life after transplant, our dedicated Patient Services team have information and support available at anthonynolan.org/patients
